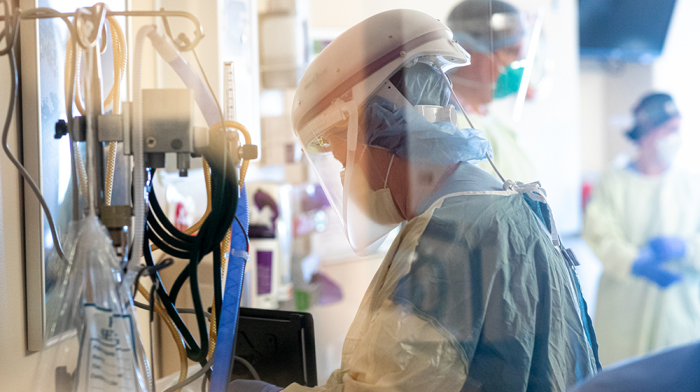
COVID-19 can ravage the human body in countless ways, making recovery a complex process that changes depending on the person. Since the advent of the pandemic in March, Farha Ikramuddin, MD, MHA, University of Minnesota Physicians physiatrist, has been on the frontlines working closely with patients to help them recover.
“Being a rehabilitation doctor, my job is to determine what deficits I see in both mental and physical functioning,” Dr. Ikramuddin said.
Initial consults with physical medicine and rehabilitation (PM&R) doctors determine the medical stability before an individualized care plan is conceived, with an end goal of discharge always in mind. Dr. Ikramuddin and colleagues, as part of the Acute Post COVID care team, met every day to discuss patients on an individual basis. COVID-19 patients’ unique complications necessitated this approach, especially since there was such a lack of knowledge regarding the virus at the time.
There were many nuances that required us to focus on each of these patients separately. For me, as a clinician who is seeing these patients from the ICU to discharge, rehabilitation is a very important aspect of their recovery and continuity of care. I feel very honored and privileged to see how they’re making their recovery.
Dr. Farha Ikramuddin
Many COVID-19 patients were intubated for four weeks or more — an unusually long time considering most patients spend just a single week in similar critical care settings. This is unique to COVID but a necessary part of their treatment. Specifically, intubation in a prone position leaves the patients sedated. This can have a significant and detrimental effect on muscles throughout the body, in addition to the effects of the virus itself.
“The muscle atrophy that I have seen since March is probably something that I will carry the rest of my life. I don’t think I’ll see that again. There are a lot of systemic factors that lead to their function being impaired,” Dr. Ikramuddin said.
Some of this impairment is due to the prolonged sedation and ventilator care that patients require to survive. In addition to muscular atrophy, patients with severe COVID-19 sustain injury to their kidneys, liver, brain and other organs. Other complications include stroke, bleeding in different muscle groups and pulmonary embolism, which causes a clot in the lungs that affects oxygenation — an obviously dangerous development when you’re already dealing with respiratory issues. The neurological after-effects can also be profound and sometimes irreversible, so physicians like Dr. Ikramuddin regularly monitor cognitive functioning.
Roughly a third of COVID-19 patients experience dysexecutive syndrome, meaning there is impairment of executive functions and possible permanent impairment to their cognition. Previous data from acute respiratory syndromes, such as sepsis, demonstrate the importance of following these patients after their recoveries.
We have so many systems in place that establish checkpoints to make sure that nothing is falling through. I would like to follow the patients long term to determine the overall prognosis and to learn more. As we see the surge again both nationally and locally, we have formed the Acute Post Huddle again to best serve the needs of our patients.
Dr. Ikramuddin