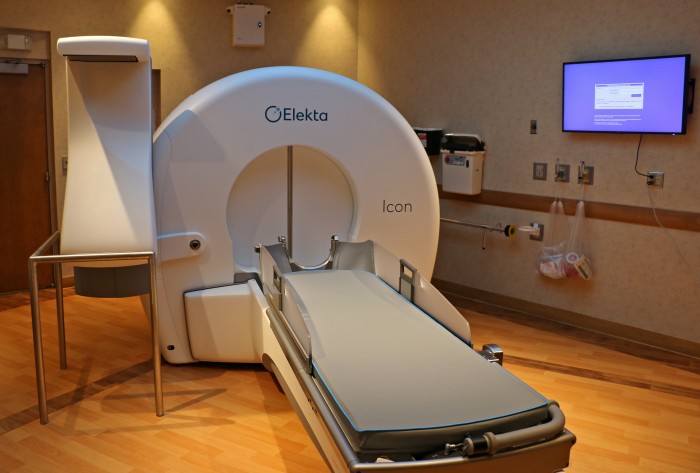
The University of Minnesota Medical Center is the first location in the state to treat brain tumor patients with the latest generation of advanced radiosurgery technology, the Gamma Knife Icon. “We are the only health care system in the state of Minnesota to offer treatment using the new Gamma Knife Icon,” says University of Minnesota Physicians Radiation Oncologist Kathryn Dusenbery, MD. “Bringing the new technology to the medical center was certainly a team effort that included our radiation specialists, neuro-oncologists, neurosurgeons, and medical physicists.”
The technology has been available for 14 years but the Gamma Knife Icon is the sixth generation of Gamma Knife radiosurgery machine. It is capable of targeting treatment areas with accuracy to within 0.15 millimeters, or the width of two human hairs, the most accurate of the Gamma Knife machines to date.
Radiosurgery is an advanced form of radiation treatment that delivers high doses of radiation to a tumor without exposing the surrounding brain tissue. It works by focusing radiation beams from different angles on a small target. While each beam delivers a small radiation dose that is well-tolerated by the brain, the point where the beams converge receives a high dose that is sufficient to eradicate tumor cells.
Clark Chen, MD, Lyle French Chair and Head of the Department of Neurosurgery at the University of Minnesota Medical School, explained, “For this radiosurgery to work, precision of radiation delivery is essential. Being off by a few millimeters can mean the difference between destroying tumor cells and mutilating normal brain.”
The older version of Gamma Knife required usage of a metal headframe that was affixed to a patient’s skull to immobilize the treatment area. Now, clinicians have the opportunity to perform procedures using an individualized molded, mesh-style mask, an option that improves the patient experience.
“In radiosurgery, we don’t expose patients to the possible downside effects of treating their whole brain,” stated Dusenbery. “With the Gamma Knife Icon, we treat such a small area of the brain and the rest of the brain gets so little dose that patients don’t lose their hair and neurocognitive decline is not a concern.” Radiosurgery is particularly beneficial for patients afflicted with small brain tumors or a limited number of brain tumors.
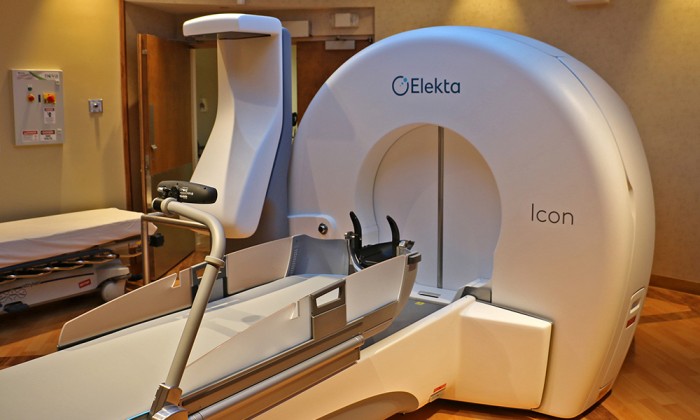
While this technology has benefits, Chen cautioned, “In patients who have a small target or require high radiation doses, the headframe still gives us the most accurate way to deliver radiosurgery and avoid radiation to the uninvolved brain. Judicious decision between frame-based or mask-based radiosurgery will require a multi-disciplinary discussion between radiation oncology and neurosurgery.”
Patients have already been utilizing the Gamma Knife Icon since June 24. It’s yet another example of the tremendous care available from M Physicians’ clinicians.
We are the only health care system in the state of Minnesota to offer treatment using the new Gamma Knife Icon.
Kathryn Dusenbery, MD, University of Minnesota Physicians Radiation Oncologist